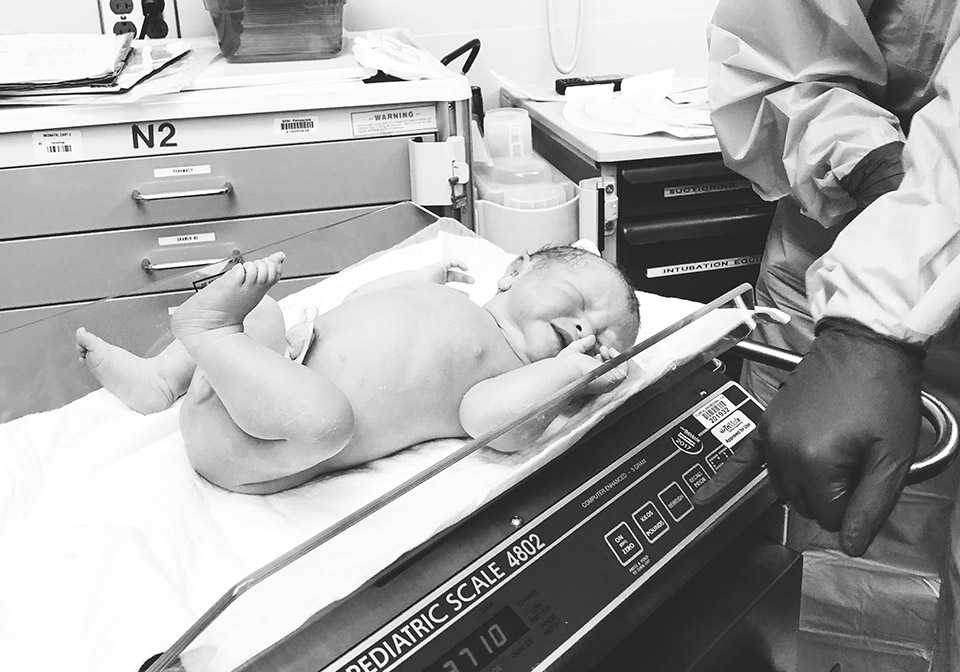
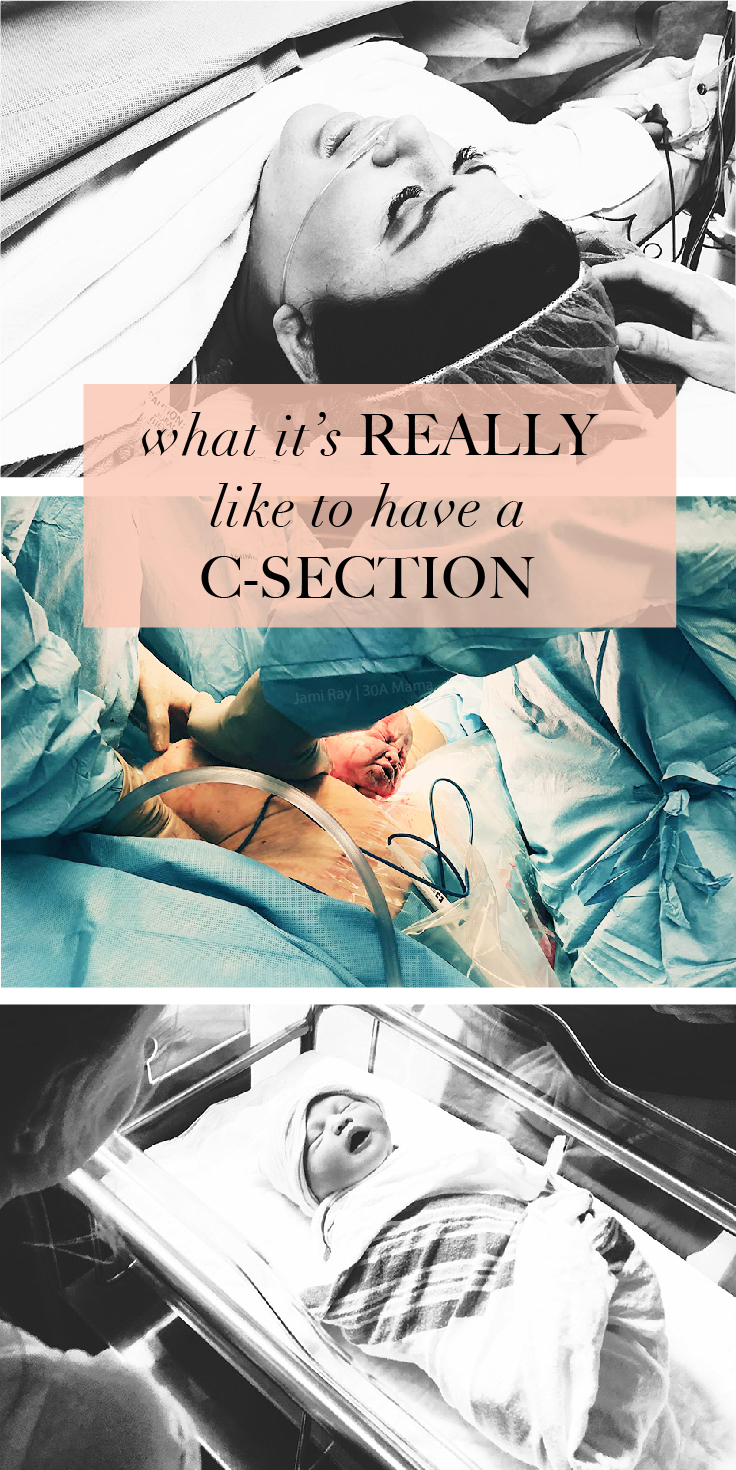
I remember the moment I opened the calendar app on my phone and tapped out the appointment for the C-section that would deliver my sweet Collins. By the time I reached those final weeks of the third trimester, I was more than ready to meet the baby and loved having a set day and time to look forward to. It felt so surreal and exciting, yet scary and uncertain at the same time.
Did you know around one third of babies delivered in the US arrive via C-section? Interestingly enough, this number has grown steadily over the past few years as more women opt for this procedure over natural delivery or undergo an emergency C-section due to complications or other medical reasons. Like my first pregnancy with Emery, I knew with Collins that labor wasn’t for me and I would be one of the “C-section moms” once again. Even though I’d been through this the first time, my experience with Collins still felt new, partly because of the six year gap and partly because these details just aren’t that talked about. It’s almost as if the baby’s arrival creates such a happy fog and shifted focus to the little one, that our experience and what happens to our body is all but forgotten. Someone in the OR (I think it was the nurse anesthetist?) offered to take photos on my phone and I couldn’t be more grateful to have these snapshots. As one of the many moms with a scar to show for it, I wanted to share what it’s really like to have a C-section.
A C-section isn’t the easy way out.
A C-section is an intense abdominal surgery that comes with plenty of pain and some serious recovery time. It involves cutting an incision through both the stomach and uterus to deliver the baby, which can be even riskier than natural delivery. While there may be a few who request a C-section as a way to avoid the effort of labor, that’s certainly not the case for everyone. Because of a congenital heart condition that put me in the high-risk category and presented potential complications with labor, my doctors including my OB/GYN and cardiologist strongly advised against laboring so that I would be in the safest, most controlled cardiac environment. It’s just the hand I was dealt because of my medical history. It wasn’t a luxury decision to simply “wake up with a baby” – a misconception I’ve actually heard first hand.
First, there’s paperwork.
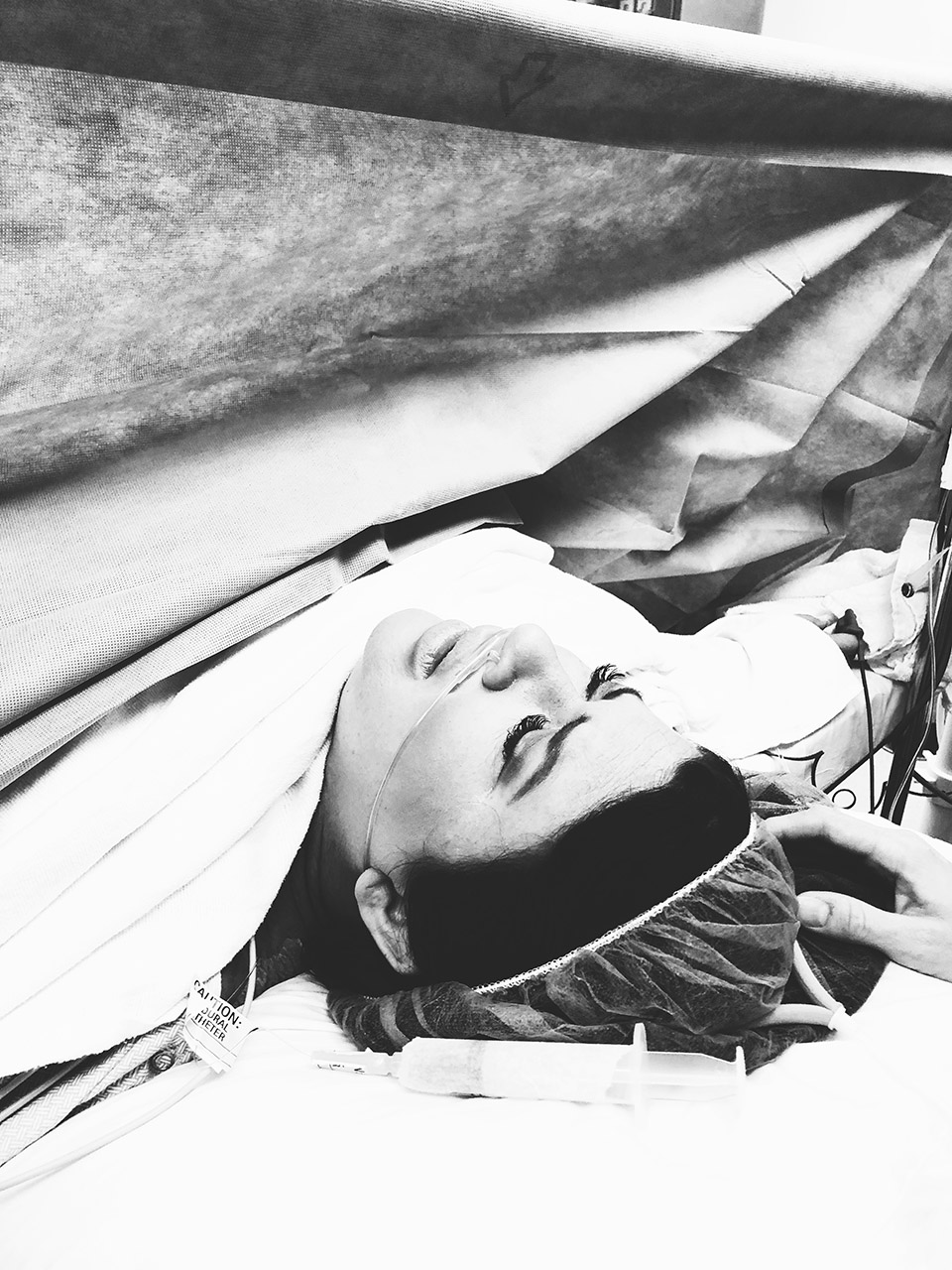
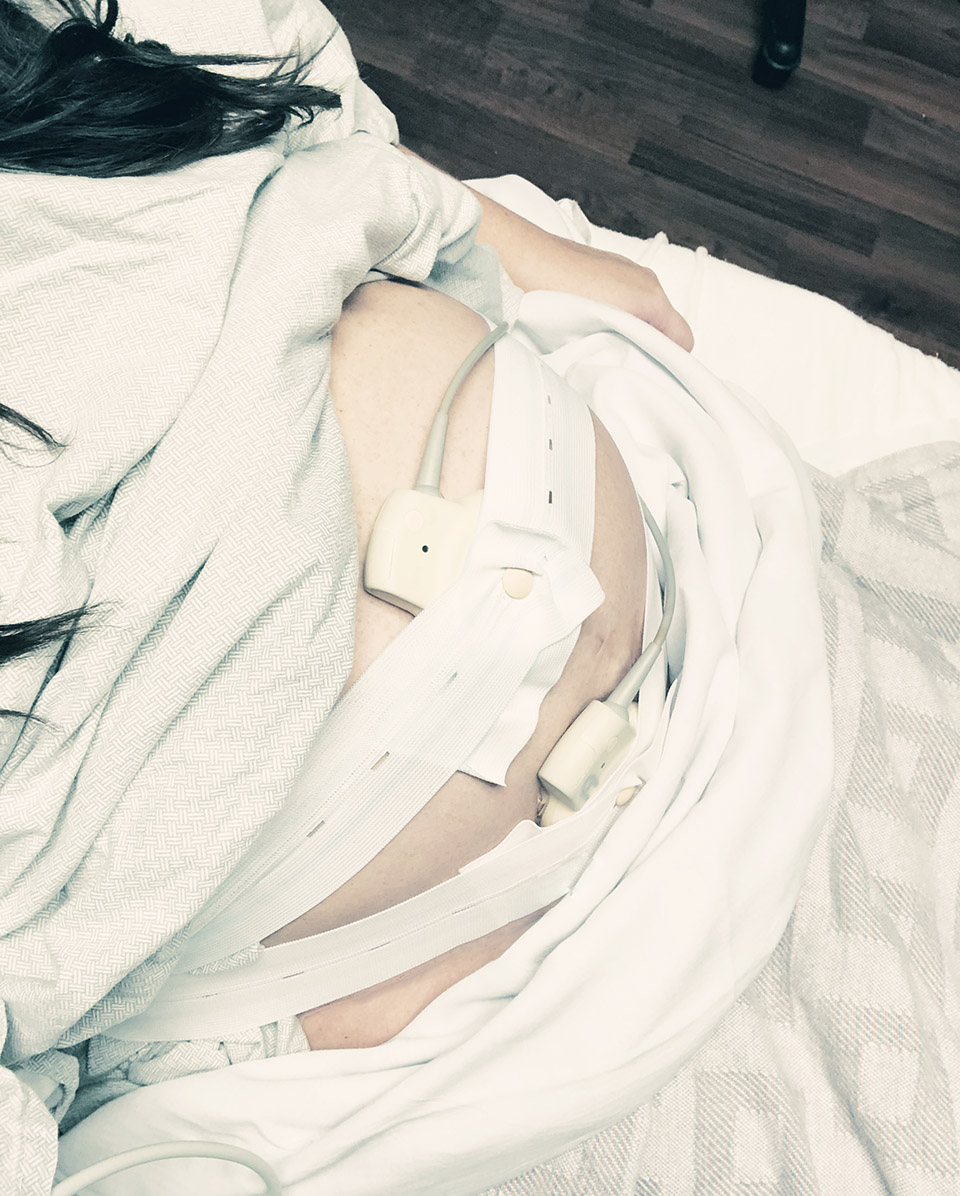
Even with a scheduled date and time, there is still a lot to check off the list before being wheeled into the OR. As soon as we checked in, I changed into the super stylish hospital gown and socks waiting for me. There’s always a ton of paperwork and prep, which we started filling out right away. Do I understand the risk? Do I want the placenta? Do I want to donate the placenta? Do I want skin on skin immediately after? As with most surgeries, no food or drink was allowed after midnight the night before, which meant an afternoon “appointment” left me starving. I was given a not-so-pleasant drink to help dry oral secretions during the surgery. The nurses insert an IV to take blood and later administer medicine and fluids as needed. The team of doctors and the anesthesiologist come in to introduce themselves and go over what will happen. The nurses make sure the incision area is prepped and shaved (if you didn’t arrive with that done) and put a catheter in place.
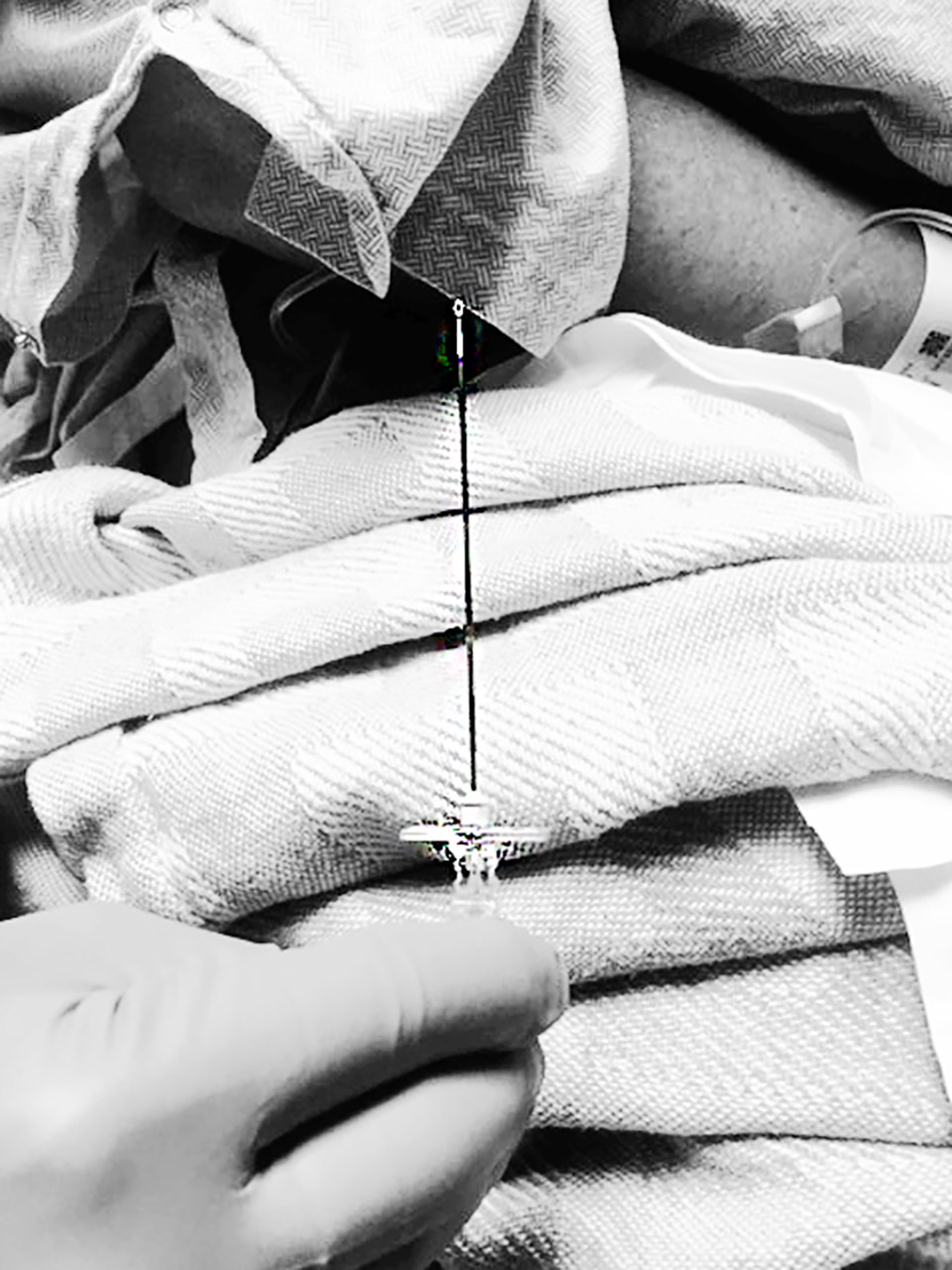
The epidural can be tricky. And it hurts like a !*$%.
The size of the epidural needle is impressive on its own. Since I had to be completely under when Emery was born, I didn’t get a full look at the whole epidural “kit” until this time around. The feeling of the doctor pressing around to find the exact point on my spine to insert the needle was nearly excruciating in anticipation of what was coming next, but the actual insertion of the needle into my back was the worst pain I can remember. It doesn’t hurt once it’s in, though the feeling is a strange sensation of being aware something’s there, but not really feeling it. My epidural was given in the prep room because I had a history of it being difficult, though they are often given in the OR as well. Once I had the epidural, I was ready to start receiving the medicine to numb my lower half. As they loaded in the first dose, I had a fast reaction to the anesthesia and immediately felt sweaty, lightheaded and loopy, so they quickly gave me additional meds to counteract the reaction. Because of this, the team decided to slowly load in the full dose instead of sending it through at the usual rate. Apparently my body reacts strongly to drugs! This took a little while to get up to the full dose and I actually fell asleep during this process, though normally, it would progress from this point pretty quickly.
You’re wheeled into the OR alone.
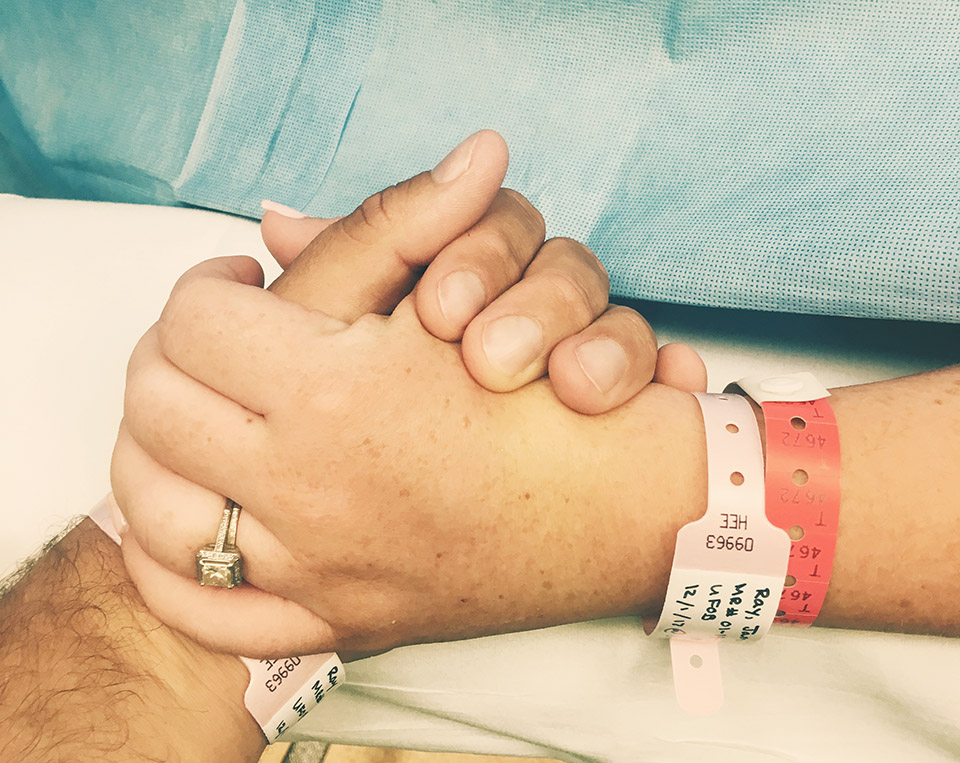
Once my reaction was stabilized and my dosage was up to the full level, the anesthesiologist checked for feeling on my stomach and legs and we were off to the OR. Hunter was given a set of scrubs and shoe covers to wear in the OR, but wasn’t allowed to come in until everything was set. Both of our families were there in the prep room up to this point and as we kissed and I was wheeled out, they were all moved to the waiting room. By this time, I was feeling nice and a little fuzzy – still alert, but also aware that I couldn’t fully feel my lower body. Inside the OR, the team moved me from the bed onto the surgery area where my arms were stretched and secured to each side like a T. Since I hadn’t eaten in so long, I had to have glucose to raise my blood sugar to a satisfactory level. As the team draped and brushed my stomach with an antiseptic, a screen was placed in front of my chest and the anesthesiologist tested different pressures to see if I was ready. When I couldn’t feel anything, it was time for the surgery and Hunter was allowed in the room to hold my hand.
The C-section pressure feels SO weird.
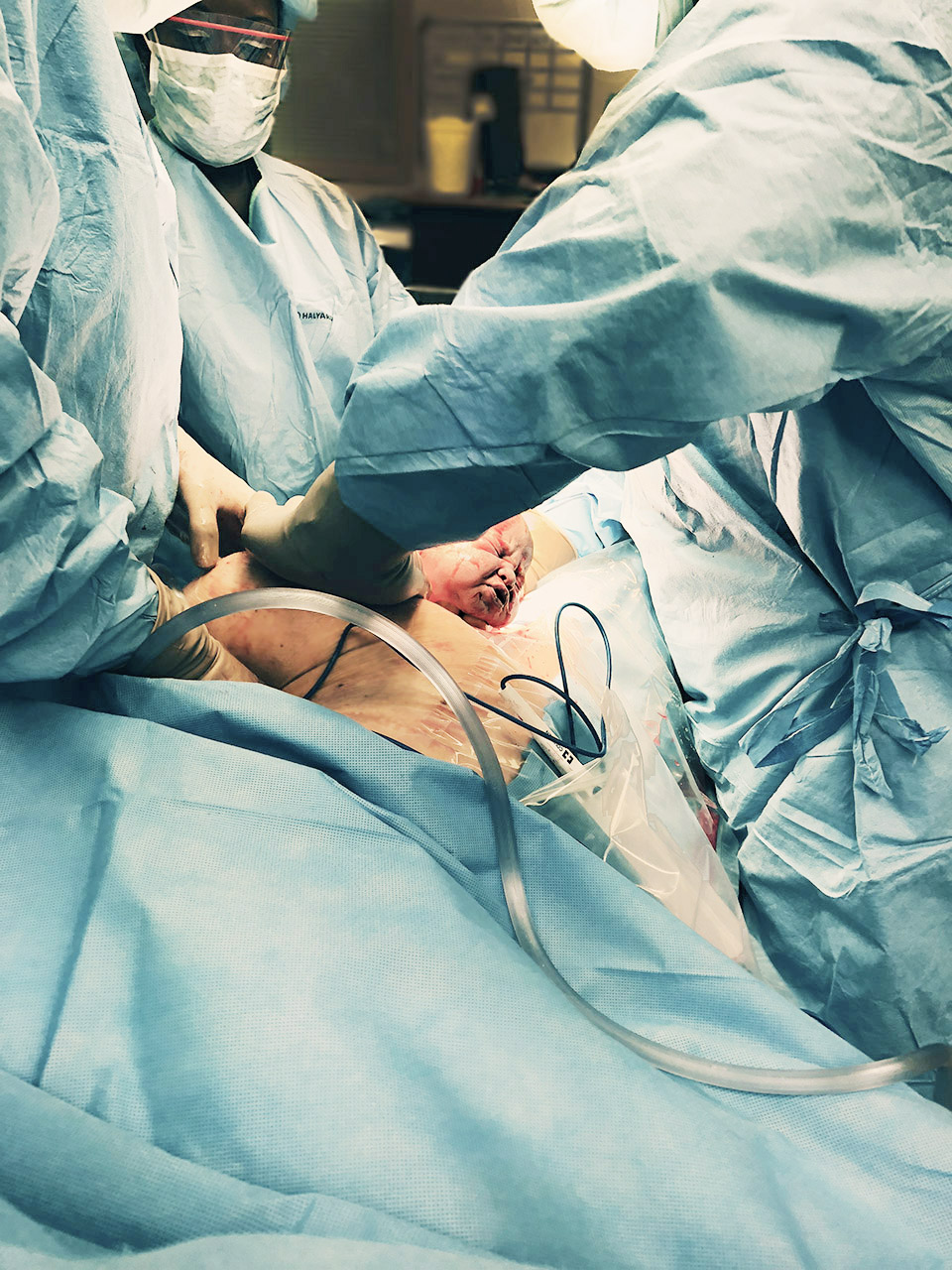
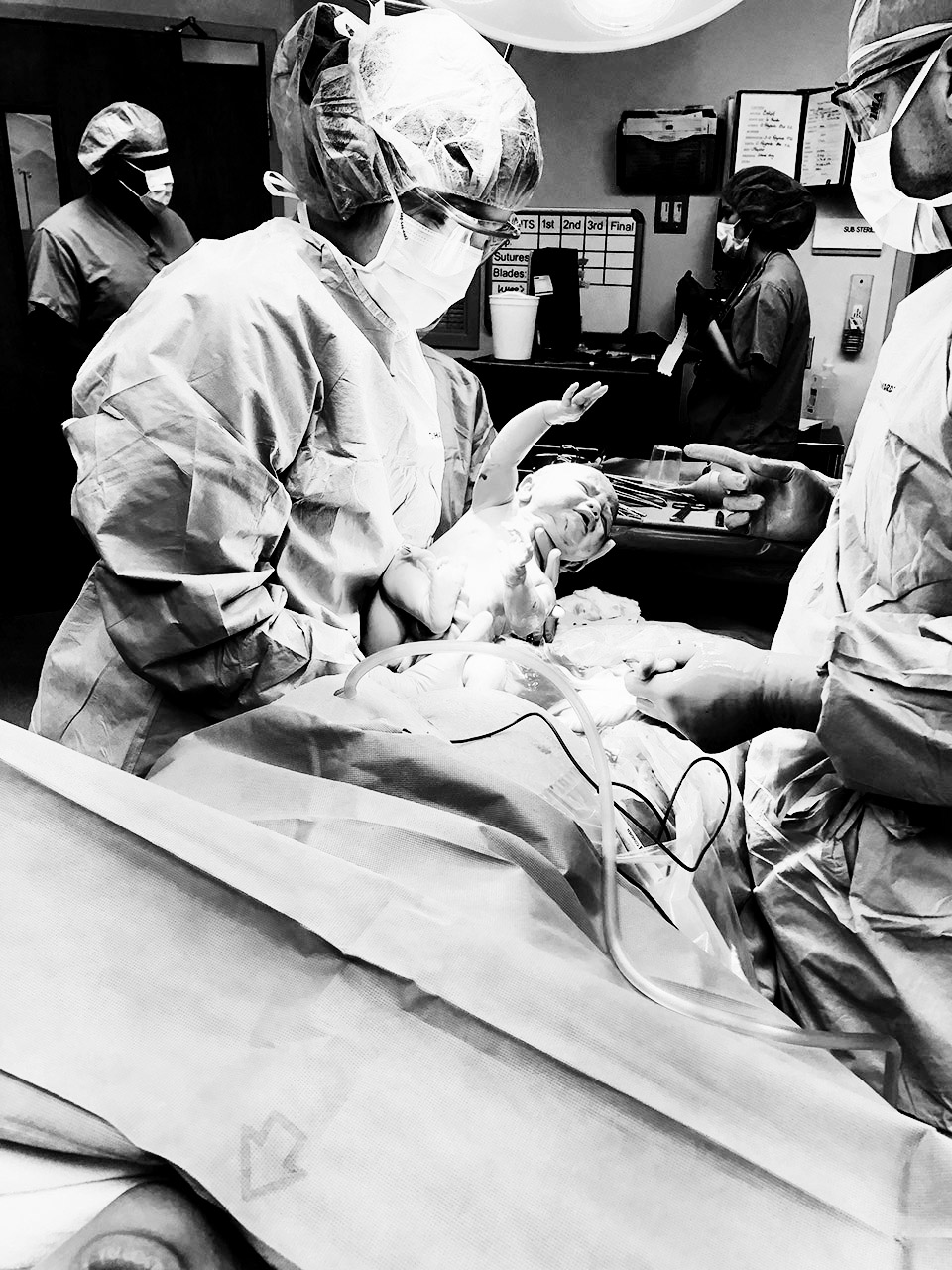
I was warned that I would be able to feel that something was happening in my abdomen area, but that I wouldn’t feel pain. It was described as an intense pressure and honestly it is the strangest feeling that I’m not sure “pressure” adequately describes. I didn’t feel a thing when the incision was made, but as they made progress and announced each step, the feeling changed. The doctor said to prepare for a heavy push and it felt like my insides were being pulled completely out of my body. This part involves both pulling the baby out from the incision and simultaneously pushing my stomach from the top downward. It was the hardest part for me and that exact moment is pictured a few photos below. In my head I imagined a car tire running over my stomach, though it was more of a distant pain because I knew what was happening but I couldn’t fully feel the impact.
The actual delivery happens fast.
According to the time stamps on my phone, I left the prep room at 7:41 pm and Collins took her first breath at 8:11 pm. That’s exactly 30 minutes to get into the operating room, have final preparations on the table, receive more meds through the epidural, have the incision made and the baby pulled out. It’s both methodical and mind-blowing. Beware, the next few photos are graphic.
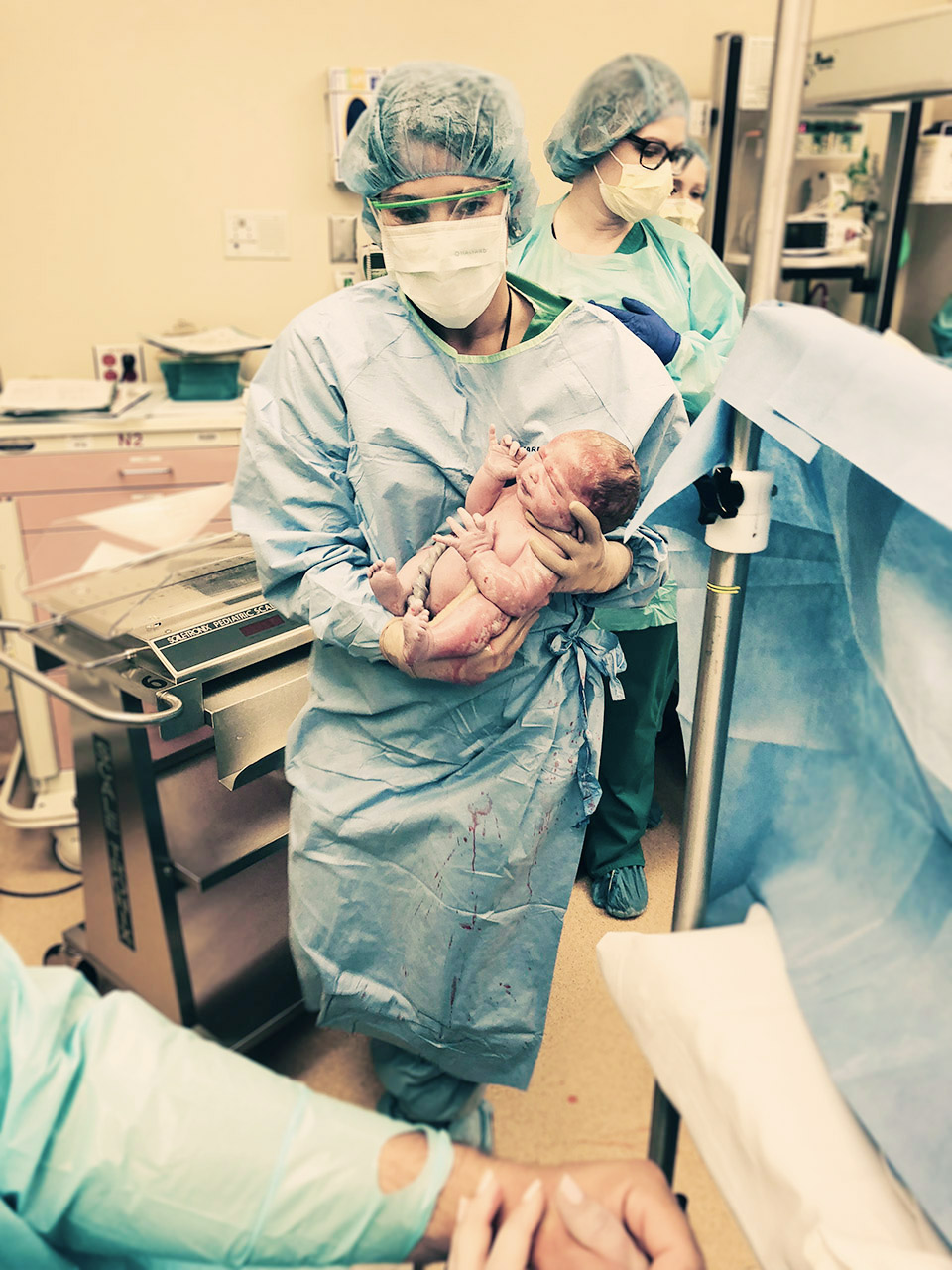
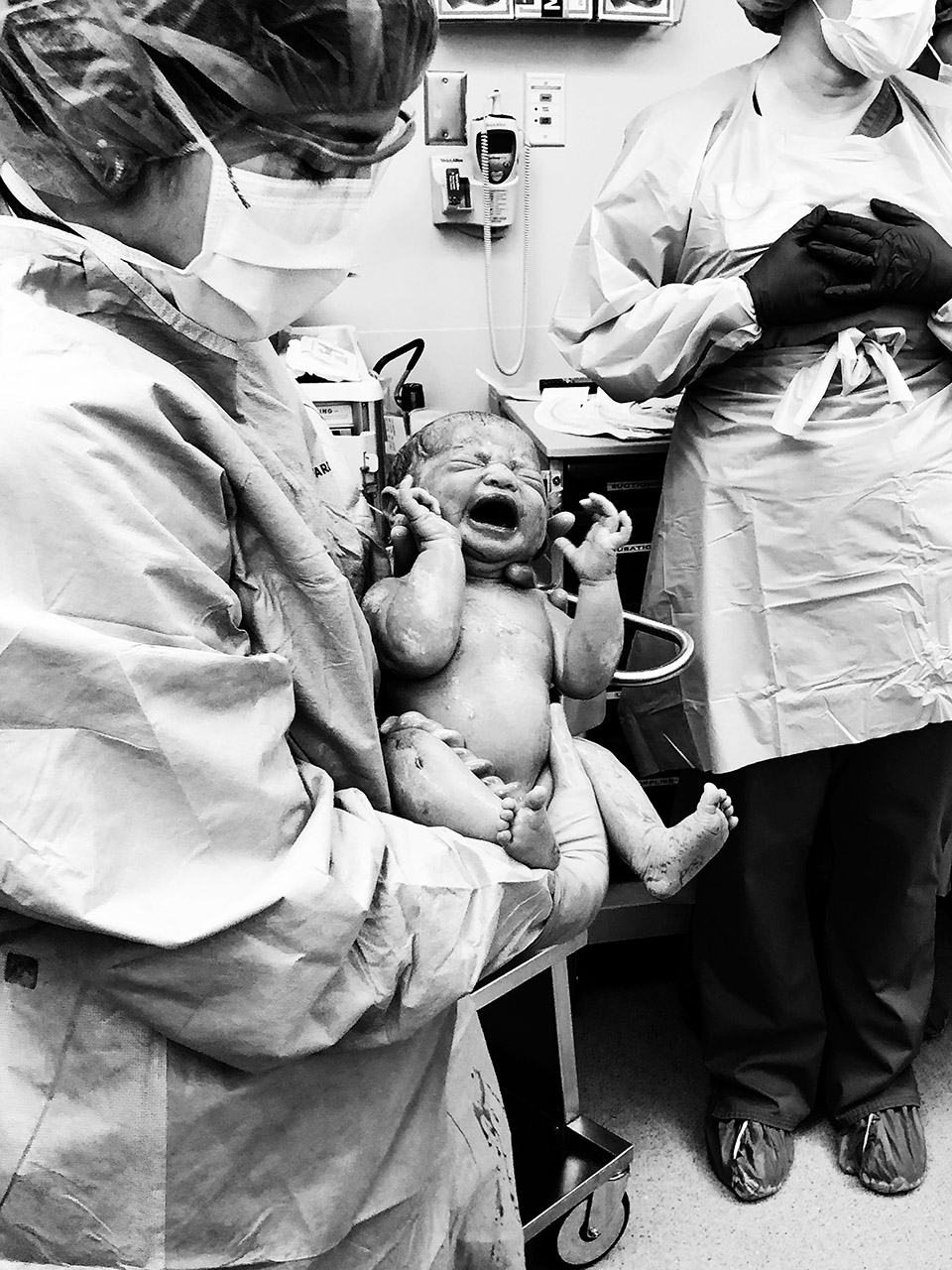
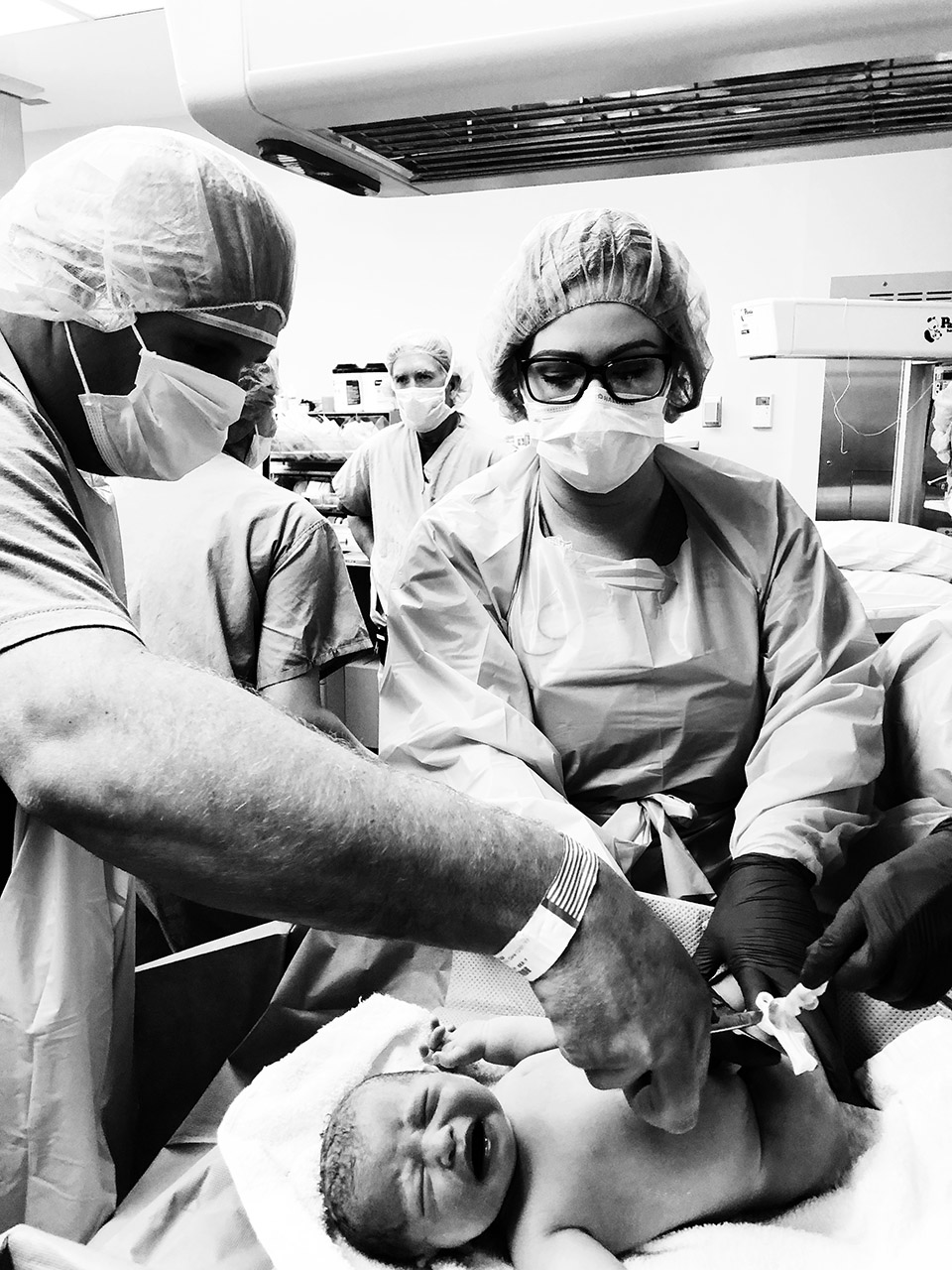
It takes awhile to put everything back together.
While Collins made her debut fairly quickly and I was able to see her right away, I had to wait until moving to post-op to hold her on my own. Meanwhile, she was taken over to one side of the room to be assessed, cleaned and measured. Hunter cut the cord and we talked about how beautiful she was and how much hair she had while the surgeons began stitching me layer by layer. That part took about 45 minutes in real time but felt like no time at all. We were already so in love with little Collie!
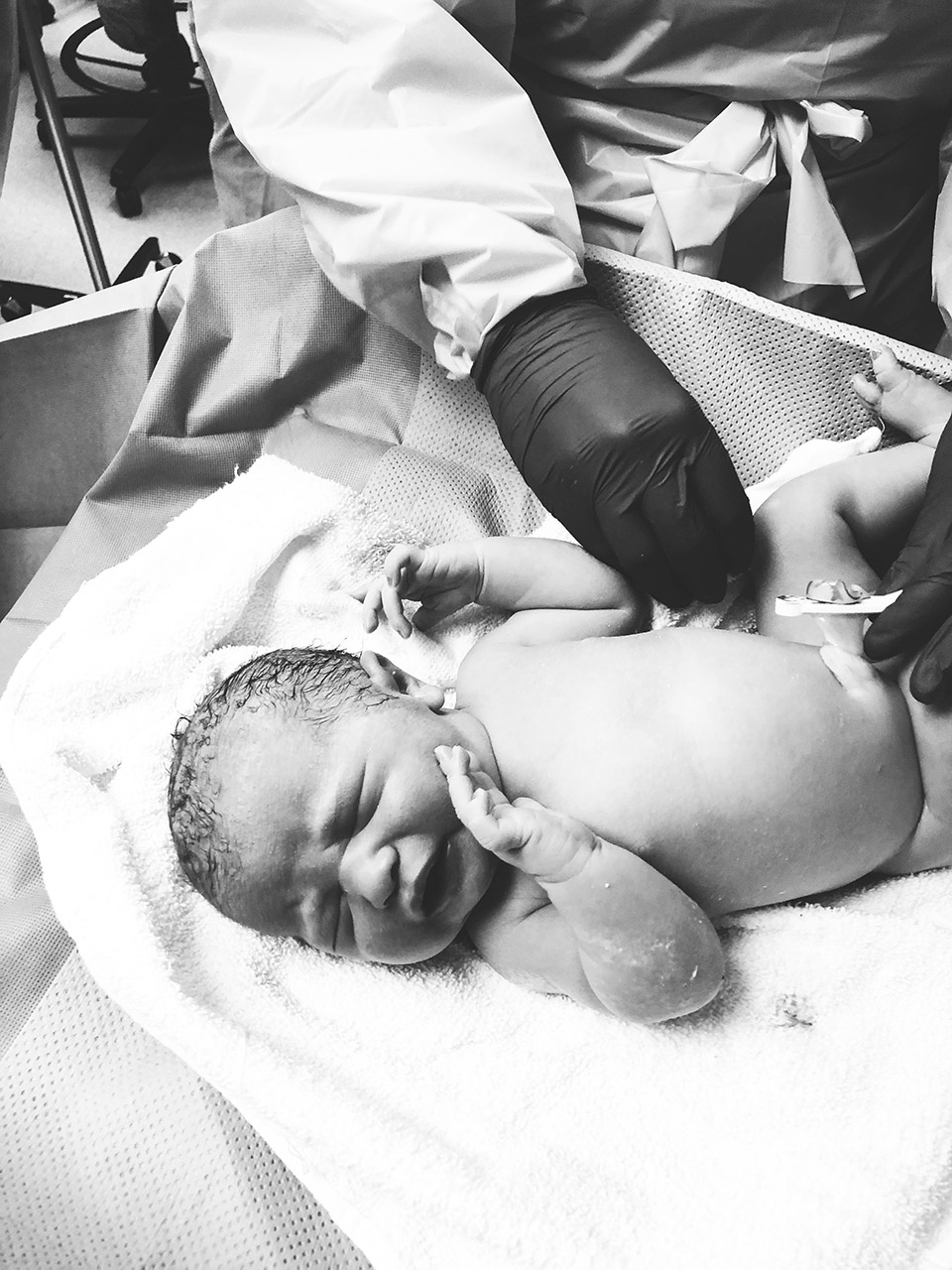
The baby love fest begins.
There’s nothing like seeing your husband turn into a proud papa to instantly melt your heart. As we did our first skin on skin and nursing in the post-op recovery area, I had an extreme feeling of deja vu. Memories of doing the same “firsts” with Emery came flooding back and I remember just how overwhelming that rush of love and emotion is. After a little time with just Hunter and me, I couldn’t wait for Emery to come in and meet her sister. I’ve never seen a bigger smile than when she held her for the first time.
The recovery…
I know, I know. This is the part no one usually wants to hear about … unless you’re going through it. After an hour in post-op, we were moved to a regular postpartum room where we stayed for 72 hours. These three days were by far the best and worst of the experience. I suggest taking full advantage of any pain meds available because the discomfort and incision pain can be nearly unbearable. I couldn’t move at all without using the buttons on the bed and even then it wasn’t advised to rise above a 45 degree angle for the first day or so. The exception to this is after 10-12 hours when they advise standing to walk to the bathroom. I was in so much pain, I couldn’t do it until nearly 24 hours after the C-section. The slightest bump, cough or muscle movement can be excruciating so I used a pillow over my abdomen when I held Collins and tried to keep my lower body as still as possible. If you’re looking at having a C-section feel free to email me for more detail about recovery.
As for the highs, having our families, particularly Emery, meet Collins was the sweetest thing to see. Emery picked out a special gift for little sis and had even practiced how to hold a baby. I had forgotten just how small and delicate babies can be, so I think that helped me savor each of those first moments even more.
Every mother’s experience with delivery is different and specific to her wishes, medical history, doctor’s advice and baby’s physical condition. C-sections are not always a first choice, but may be an only choice to deliver a healthy baby to a healthy mom in the safest situation possible. I’m happy to have made it through twice and when I think of my babies and their births, I’m reminded just how incredible life can be, with or without a scar.
I’d love to hear from you! If you had a C-section, what do you remember most? If you were able to deliver naturally, what were the best and worst parts?
Add this post to your Pinterest board to save for later.